Clinical utility of circulating tumor cells in patients with non-small-cell lung cancer
Introduction
Experimental evidence suggests that dissemination of tumor cells is an early event in the progression of solid tumors (1). Through a process called epithelial-mesenchymal transition (EMT), cancer cells acquire the ability to invade the basal membrane and to enter the systemic circulation. Disseminated tumor cells (DTC) have indeed been identified at early stages of tumor progression in regional lymph nodes, peripheral blood, and in bone marrow of cancer patients using highly sensitive detection methods. In this respect, the term DTC refers mainly to cells that home in the bone marrow, whereas circulating tumor cells (CTC) are rare tumor cells that can be isolated from the peripheral blood (2). Only a small fraction of CTC will eventually form a metastasis at distant organs, where tumor cells regain the epithelial phenotype (mesenchymal to epithelial transition, MET).
Identification of CTC can provide relevant prognostic and predictive information (Figure 1). CTC might allow early detection of tumor development in high-risk individuals. In patients with limited, surgically resectable disease the presence of CTC might suggest a metastatic spread, thus providing information that could help to guide treatment decisions before the onset of overt metastases. The levels of CTC have been shown to be associated with prognosis in different malignancies, in which they reflect the tumor burden and the biological aggressiveness of the disease (3). CTC variation during systemic treatment of patients with metastatic disease treatment has also been shown to reflect drug sensitivity. Finally, molecular characterization of CTC might provide new insights into the mechanisms of tumor metastatization and allow identifying actionable genetic alterations.
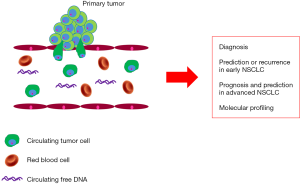
All the above potential applications of CTC detection have been explored in non-small-cell lung cancer (NSCLC). NSCLC is the most frequent form of lung cancer, accounting for approximately 85% of all lung cancers (4). Diagnosis of NSCLC occurs frequently in advanced stage of the disease and, therefore, the prognosis of this tumor is extremely poor (5). In this respect, biomarkers that might allow early detection of NSCLC, assessment of prognosis and identification of potential targets for therapeutic intervention are definitely needed in order to improve the prognosis of this deadly disease.
This review article will summarize the different applications of CTC in NSCLC, from early diagnosis to risk assessment in patients with early or advanced NSCLC. By doing this, we will try to draw a complete picture of current and future developments of CTC research and clinical applications in NSCLC.
CTC as a diagnostic marker in NSCLC
Because tumor cell dissemination is a relatively early event in cancer progression, identification of CTC might allow early diagnosis of NSCLC. To this end, it is mandatory to demonstrate that the detection method employed to identify CTC is able to discriminate between healthy subjects, individuals with non-malignant lung disease and lung cancer patients.
Several studies have addressed the potential of CTC identification in the diagnosis of NSCLC. These studies used different approaches, based on either the identification of epithelial cell markers in the cellular fraction of peripheral blood or the isolation and characterization of putative epithelial cells.
Sheu and collaborators (6) found that a 17-gene membrane array-based assay could detect circulating cancer cells in 90% of NSCLC patients at different stages of disease and in 6% of healthy controls. The test was positive also in 3/20 breast cancer patients, 3/15 colorectal cancer patients and 2/12 gastric cancer cases. The sensitivity of the assay was significantly correlated with the presence of distant metastases and disease stage, with the lowest sensitivity (78.8%) found in stage I patients.
Different studies have used the folate receptor transcript as a marker to identify the CTC (7-9). In fact, folate receptor is often expressed in NSCLC cells whereas its levels of expression are usually low in blood cells. These studies have shown that by using folate receptor as a marker it is possible to discriminate between NSCLC patients, individuals with benign lung disease and healthy subjects. A sensitivity up to 77.7% and a specificity up to 89.5% for the diagnosis of NSCLC was reported (7,9). However, it must be emphasized that the sensitivity was higher for stage IV patients, while it was <70% in stage I.
The isolation by size of epithelial tumor cells (ISET) technology coupled with cytomorphological evaluation of isolated cells can allow the identification of CTC, which have been also defined as circulating non-hematologic cells (CNHCs). ISET identified CHNCs with malignant features at a significantly higher frequency in patients with malignant disease as compared with subjects with non-malignant pathologies (10). By using this approach, Ilie and coworkers (11) examined the presence of CTC in 168 patients with chronic obstructive pulmonary disease (COPD). These patients had no clinically detectable lung cancer and the presence of CTC was explored in complement to CT scan for early lung cancer diagnosis. CTC with malignant features were detected in 5/168 patients (3%) of COPD patients. CT-scan screening detected lung nodules 1 to 4 years after CTC detection in all CTC-positive COPD patients. Histopathological diagnosis following surgical resection confirmed the diagnosis of early-stage lung cancer. The patients were without tumor recurrence and without CTC 16 months after surgery thanks to this early diagnosis. Importantly, patients with COPD without CTC (n=160) as well as patients with CTC with benign features (3/168; 1.8%) did not develop lung nodules during the follow up. Although preliminary, these findings confirm the potential of CTC detection for early diagnosis of NSCLC in patients at high risk to develop lung cancer.
More recently, a size-based microfluidic chip for detecting single CTC and CTC clusters allowed for the detection of CTC in lung cancer patients with apparent high sensitivity and specificity when compared to healthy controls (82.7% sensitivity and 100% specificity) (12). Interestingly, the levels of CTC in stage I–II patients were lower as compared with patients in advanced stage or with local recurrence of the disease, thus reinforcing the need for high sensitive techniques for early diagnosis of lung cancer through CTC detection.
Detection and prognostic value of CTC in early NSCLC
Although the number of CTC generally correlates with tumor stage, CTC can be detected in early NSCLC. A number of studies have addressed the role of surgical manipulation on the dissemination of CTC as well as the prognostic significance of CTC detection before and/or after surgical resection of lung tumors.
It has long been hypothesized that any manipulation of the tumor mass might facilitate the release of tumor cells in the bloodstream, although the implications of this phenomenon in the dissemination of the disease have not been elucidated. In this respect, a recent study analyzed CTC in peripheral vein blood samples obtained before and after lung tumor biopsy using flexible fiber-topic bronchoscopy. In 2/6 patients, CTC were absent before bronchoscopy but they were detected after lung biopsy (13). In early lung cancer, CTC can be detected in the pulmonary vein (PV) blood in addition to the peripheral blood. A number of studies have shown that the levels of CTC are usually higher in PV blood samples as compared with peripheral draws, suggesting that CTC might be in part removed by the circulation after shedding from the tumor mass (14-17). Interestingly, Reddy et al. found that PV CTC were more frequently detected in patients who underwent preoperative bronchoscopic biopsy (8/9 cases), compared with patients who underwent CT-guided biopsy (4/12) (16). Although the limited number of patients included in these studies prevents any firm conclusion, these findings confirm the possibility that biopsy of tumor mass might lead to tumor cell dissemination.
Surgical manipulation of the primary lung tumor might also contribute to CTC dissemination. In this respect, Hashimoto and collaborators (15) found that the median number of CTC in PV samples increased from 4 to 60 in 30 consecutive primary lung cancer patients who underwent lobectomy through open thoracotomy. An increase in CTC during and/or after surgery has also been observed in studies that assessed peripheral blood samples using different detection methods (18-21). Interestingly, CK19 and CEA transcripts have shown a different peri-operative kinetic when used as markers of CTC dissemination (20). The value of CK19 mRNA during the operation was significantly higher than that of pre-operation and post-operation; in contrast, the post-operative levels of CEA mRNA were significantly higher than those of pre-operation and those of operative day. Because CK19 mRNA is expressed in all epithelial cells, this might indicate that surgery leads to release of CK19 mRNA from non-transformed cells and, therefore, it might be not an adequate marker for CTC detection.
The correlation between surgical techniques and CTC dissemination has been also explored. Hashimoto and collaborators (15) reported that the increase in CTC count after surgery was not significantly associated with the sequence of vessel interruption (pulmonary artery first versus PV first). In contrast, Ge and co-workers (20) found higher levels of CEA mRNA in patients had the ligation of the pulmonary artery first as compared with PV first. However, it must be emphasized that no difference in survival using different sequences of pulmonary vessel ligation has been described (18). A more frequent increase in CTC has also been reported in patients undergoing limited resection as compared with pneumonectomy (22), as well as in those receiving video-assisted lobectomy as compared with open lobectomy (18).
Taken together, these studies have shown that surgical manipulation might indeed induce CTC dissemination. However, the observation that CTC can be detected before surgical manipulation in selected early NSCLC patients, suggests that tumor dissemination might precede surgical intervention. In this respect, the above summarized studies did not provide a formal demonstration that the surgical techniques might affect patients’ prognosis through CTC dissemination.
A number of studies have addressed the prognostic value of CTC detection in early NSCLC (Table 1). Different mRNA markers have been employed to track CTC in the peri-operative period in patients undergoing surgical resection of primary NSCLC with curative intent. In a prospective study of 103 consecutive NSCLC patients who underwent a curative lobectomy, pre- and post-operative CEA mRNA levels were assessed in peripheral blood samples (23). At multivariate analysis, lack of CEA mRNA expression was an independent prognostic factor for overall survival (OS) with a hazard ratio (HR) of 0.21. Yie and collaborators (24) evaluated the levels of expression of survivin in pre-operative peripheral blood samples obtained from 67 stage I-III NSCLC patients. With a median follow-up period of 18 months (range 3–36 months), the detection of survivin-expressing CTC was found to be an independent negative predictor for cancer recurrence (HR 43.5) and survival (HR 1.35) at multivariate analysis. Thyroid transcription factor-1 (TTF-1) is expressed only in epithelial cells of the thyroid and in bronchioloalveolar cells of the lung. Because expression of TTF-1 is frequent in lung adenocarcinoma (31), its expression has been used to identify neoplasms with a pulmonary origin. In this respect, the CTC status in pre- and post-surgery peripheral blood samples from 79 early NSCLC patients was investigated using TTF-1 and CK19 mRNA markers (25). The presence of post-surgery TTF-1 positive CTC was the strongest prognostic markers, resulting associated with earlier disease progression (P=0.004) and shorter progression-free survival (PFS) (P=0.004) at univariate analysis. In addition, patients with post-surgery TTF-1 positive CTC—but not pre-surgery—showed shorter PFS than other patients (P<0.001). However, these findings were not confirmed at multivariate analysis. Assessment of CTC at multiple time points might increase the predictive value of the assay. Li and collaborators (26) assessed the CTC status in 68 stage I-III NSCLC patients before surgery, after surgery and after completion of adjuvant chemotherapy. The LUNX mRNA whose expression is strictly limited to normal lung tissue and NSCLC was used as marker. Patients with LUNX mRNA-positive CTC at 3 time points had a shorter DFS and OS than those with positive pre-operative samples but negative post-operative and post-adjuvant therapy samples. Multivariate analysis confirmed that the presence of LUNX mRNA-positive CTC either after surgery or after the completion of adjuvant therapy were independent factors for worse DFS (HR 2.14 and 2.17, respectively) and OS (HR 2.17 and 2.25, respectively).
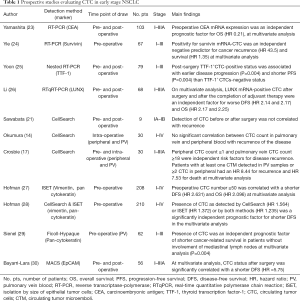
Full table
Few studies have addressed the role of CTC in early NSCLC by using the CellSearch system to isolate and detect CTC. In a small study by Sawabata and collaborators (21) that enrolled only 9 patients, 1 patient was positive for CTC before surgery and 3 were positive immediately after the operation. However, CTC were not detected in any of these patients 10 days after surgery. With a median follow-up of 14 months, no cancer recurrence was observed in any of the cases. The CellSearch was also used to detect CTC in the peripheral and PV blood samples of 30 consecutive lung cancer patients who underwent thoracotomy (14). Both peripheral and PV CTC status did not correlate with recurrence of the disease observed during a median follow-up of 13 months. The limited number of patients and the short follow up period of these two studies might have significantly affected the reported results. In this respect, completely different conclusions were drawn by Crosbie and co-workers (17) who assessed the CTC and the circulating tumor microemboli (CTM) in both peripheral and PV blood from 30 patients with early NSCLC. A CTC number ≥1 in peripheral vein and ≥18 in PV samples were independent risk factors for lung cancer recurrence (P=0.01 and P=0.001, respectively). PV CTC count was also an independent risk factor for death (P=0.01). CTM were only detected in 20% of PV blood samples. Interestingly, the combination of CTC analysis in both peripheral and PV increased the predictive value of the test. High-risk patients with at least one CTM detected or ≥2 CTC in peripheral blood demonstrated a significantly shorter DFS and OS. Multivariate analysis confirmed the predictive value of combined CTM and CTC detection. In fact, in the high-risk group the HR for lung cancer recurrence and death were 8.44 and 7.53, respectively.
By using the ISET technology, CTC were found in pre-surgery peripheral blood samples from 102/208 (49%) patients undergoing curative surgery for NSCLC (27). A number of CTC ≥50 was significantly associated with shorter OS and DFS. Multivariate analysis confirmed that the presence of ≥50 CTC in the pre-operative sample was correlated with a shorter DFS (HR 2.631) and OS (HR 2.096). The same research group compared the ISET and CellSearch technologies in 210 consecutive patients undergoing radical surgery for NSCLC (28). Survival data demonstrated that patients without CTC had a significantly longer DFS compared to patients with CTC detected by either CS alone, ISET alone or both techniques. At multivariate analyses, the presence of CTC detected by either the CellSearch (HR 1.564) or ISET (HR 1.372) methods or by both techniques (HR 1.235) was an independent significant prognostic factor for shorter DFS.
Disseminated cancer cells were observed in pulmonary venous blood of 11/62 patients with resected primary NSCLC, using immunocytochemical staining of cytospins with a pancytokeratin antibody (29). Detection of CTC was an independent significant prognostic factor of shorter cancer-related survival in patients without involvement of mediastinal lymph nodes. Finally, Bayarri-Lara and collaborators (30) assessed CTC in peripheral blood samples obtained from 56 NSCLC patients who underwent radical surgery, before and one month after surgery. CTC were enriched with MACS technology and identified by immunocytochemical methods. The presence of CTC 1 month after surgery was significantly associated with a shorter DFS as confirmed at multivariate analysis (HR 5.75).
Prognostic and predictive value of CTC in advanced NSCLC
Several different studies have assessed the role of CTC count in patients with advanced NSCLC. Although the CellSearch system was the most frequently used technique for CTC detection in this setting (Table 2), several studies used different methods based either on antibody-mediated identification of CTC or expression of tumor-specific transcripts (Table 3). One of the major drawbacks of CTC studies in metastatic NSCLC is that heterogeneous cohorts of patients have been enrolled. Therefore, we tried to group and discuss together clinical studies that enrolled patients with similar pathologic features and treatments.
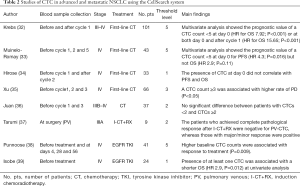
Full table
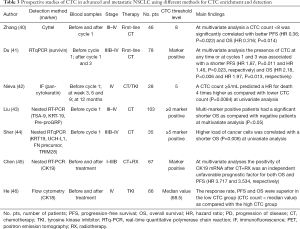
Full table
Several studies have addressed the prognostic value of CTC in chemo-naïve advanced or metastatic NSCLC patients that received standard chemotherapy as first-line systemic therapy. Krebs and co-workers assessed the prognostic value of CTC count with the CellSearch System in 101 NSCLC patients (14 stage IIIA, 27 stage IIIB and 60 stage IV) who received standard chemotherapy (32). Notably, before administration of chemotherapy only 9 patients had ≥5 CTC. Nevertheless, at univariate analysis a count ≥5 CTC before administration of chemotherapy was associated with a shorter PFS (6.8 versus 2.4 months; P<0.001) and OS (8.1 versus 4.3 months; P<0.001) as compared with <5 CTCs. The prognostic value of CTC count at baseline was confirmed at multivariate analysis (HR for OS 7.92). When the CTC levels before and after one cycle of chemotherapy were considered, a CTC count <5 at both time points was an even stronger predictive marker (HR for OS 15.65). Interestingly, a reduction in CTC count after administration of chemotherapy was also predictive of longer PFS (5.4 versus 1.9 months; log-rank test P<0.001) and OS (8.3 versus 3.3 months; log-rank test P<0.009) (32).
A prospective trial of 43 stage IV NSCLC patients confirmed at univariate analysis that a CTCs count ≥5 before administration of first-line chemotherapy correlated with worse PFS and OS (P=0.034 and P=0.008, respectively) (33). However, at multivariate analysis only the correlation of CTC count with PFS was statistically significant (HR 4.3; P=0.016). An exploratory analysis also suggested that an increase of CTC count after chemotherapy was predictive of progressive disease and shorter PFS (33).
In contrast, the prognostic value of CTC count with the CellSearch system was not confirmed by Hirose and collaborators (34). Among 33 chemo-naïve stage IV NSCLC patients, 12 (36.4%) had at least 1 CTC in the peripheral blood and 5 (15.2%) had ≥5 CTCs. Patients with one or more CTC showed an higher rate of progressive disease (66.7%) as compared with CTC-negative patients (23.8%; P=0.02) following chemotherapy treatment. However, the presence of CTC did not correlate with PFS and OS (34).
The correlation with survival of CTC counts was not reported by Xu and collaborators, who identified peripheral blood CTCs in 47/66 (71.2%) chemo-naïve stage IV NSCLC patients by using the CellSearch (35). However, they found that the number of patients with ≥3 CTCs decreased significantly after two cycles of chemotherapy. In this respect, a count ≥3 CTCs after two cycles was associated with an higher rate of progressive disease (P<0.05) (35).
Two additional studies have investigated the prognostic role of CTC on chemo-naïve patients receiving standard chemotherapy using different methods for CTC count (Table 3). Zhang and collaborators used a gradient-centrifugation method (Cyttel) to investigate CTC in 46 stage III–IV NSCLC patients (40). Patients with a CTC count <8 had a better OS (21.3 versus 9 months) and PFS (7.4 versus 5.3 months) as compared with those having ≥8 CTC. Multivariate analysis confirmed the correlation between low CTC count and both PFS (HR 0.36; P=0.022) and OS (HR 0.316; P=0.014) (40).
By using survivin mRNA as surrogate biomarker for CTC detection, CTC were detected in 54/78 (69.2%) stage IIIB and IV NSCLC before administration of chemotherapy, in 41 (52.6%) after cycle 1 of chemotherapy and in 38 (50.7%) after cycle 3 (41). The presence of survivin transcripts before chemotherapy was significantly associated with shorter PFS (P=0.004) and OS (P=0.007) at univariate analysis. Multivariate analysis confirmed that the presence of CTC at any time (before chemotherapy, cycle 1 and 3) or at cycles 1 and 3 was associated with a shorter PFS (HR 1.87 and 1.46, respectively) and OS (HR 2.18 and 1.97, respectively) (41).
The prognostic value of CTC in patients receiving chemotherapy has been addressed in other studies that enrolled both chemo-naïve and pre-treated patients.
Nieva and co-workers assessed CTC by three color immunofluorescence imaging in 28 either chemo-naïve or previously treated NSCLC patients who received cytotoxic chemotherapy or EGFR kinase inhibitor (42). A CTC count ≥ 5/mL predicted a HR for death four times higher as compared with lower CTC count (P=0.0084) at univariate analysis.
CTC assessment with the CellSearch system was not prognostic in a study that analyzed 37 fragile patients (36). In fact, no significant association between CTC count and both PFS and OS was observed using a threshold of two CTC to discriminate between high- and low-CTC count.
The probability to detect CTC is increased by using multiple markers for their identification. For example, when transcripts for tumor specific antigen 9 (TSA-9), keratin 19 (KRT-19), and pre-progastrin releasing peptide (Pre-proGRP) were analyzed by nested reverse transcriptase (RT)-PCR, 113/134 (84.3%) blood samples from lung cancer patients were positive for at least one of these markers (43). Patients who were positive for more than one marker had a significant shorter OS as compared with negative patients (P<0.01). The predictive value of positivity for multiple marker was confirmed at multivariate Cox regression analysis (P<0.05) (43). However, it must be emphasized that a heterogeneous population of patients was enrolled in this study.
Sher and co-workers used homo sapiens keratin 19 (KRT19), ubiquitin thiolesterase (UCH-L1), highly similar to HSFIB1 for fibronectin (UCH-L1), and tripartite motif-containing 28 (TRIM28) as marker transcripts to investigate CTC by semi-quantitative RT-PCR in 54 patients with advanced NSCLC. The detection rate by using this approach was 72%. At univariate analysis, the presence of a high CTC load correlated with a shorter OS in the 35 stage IIIB and IV patients who received systemic chemotherapy (P=0.006) (44).
The predictive value of CTC has been explored in studies in which NSCLC patients received multimodality treatments. A small study assessed both peripheral and PV CTC in locally advanced patients who received either induction chemoradiotherapy followed by surgery or surgery alone, by using the CellSearch system (37). The patients who achieved complete pathological response after induction chemoradiotherapy were negative for PV CTC, whereas those achieving major/minor response were positive. In addition, all patients treated with surgery alone were positive for PV CTC. However, no correlation with survival was described in this study.
A fraction of patients with early or locally advanced NSCLC are treated with chemo-radiation when surgery is not feasible because of co-morbidity or for the extension of the disease. In this regard, CK19 transcript was measured by nested RT-PCR in peripheral blood from 67 stage I–IIIB NSCLC patients (6 stage I–II, 16 stage IIIA, 45 stage IIIB) before and after chemo-radiation (45). Although CK19 status before chemo-radiation did not permit correlate with survival, the patients with CK19 mRNA expression after treatments had worse OS (P<0.001) and PFS (P<0.001) as compared to those with negative CK19 expression. Positivity of CK19 mRNA after chemo-radiation was confirmed to be an independent unfavorable prognostic factor for both OS and PFS at multivariate analyses (HR 3.717 and 3.534, respectively).
Finally, CTC count has been evaluated in studies of EGFR tyrosine kinase inhibitors (TKI) in NSCLC. A single-arm phase II trial of erlotinib and pertuzumab enrolled 41 patients with relapsed or refractory metastatic NSCLC in whom CTC were assessed with the CellSearch (38). Importantly, patients were not selected for the presence of EGFR mutations. At least one CTC was identified before treatment in 28/37 (76%) patients with evaluable samples. A high baseline CTC count was correlated with response to treatment by RECIST (P=0.009) and with radiographic response (P=0.02), but not with PET response and PFS. However, a decrease in CTC count following treatment predicted a longer PFS (38).
Isobe and co-workers assessed the prognostic value of CTC in EGFR mutant patients who progressed following treatment with EGFR TKI. At least one CTC was detected in 8/24 (33.3%) cases using the CellSearch system. Patients with CTC had a significantly shorter OS as compared with those without CTC (3.0 months vs. not reached; HR 2.9) (39).
CTC were assessed by flow cytometry in 66 EGFR mutant advanced NSCLC patients (46). Patients were divided in two groups (high CTC count vs. low CTC count) based on the median CTC count of 68.5. The response rate, PFS and OS were superior in the low CTC group as compared with the high CTC group at univariate analysis (P<0.05, P<0.005 and P<0.01, respectively).
Conclusions and future perspectives
It is difficult to derive conclusions on the clinical utility of CTC count in NSCLC. An overview of the studies summarized in this article suggests that the detection of CTC has potential for early diagnosis as well as for prognostic assessment in early and advanced NSCLC. In agreement with this conclusion, a previous meta-analysis found that the presence of CTC indicates a poor prognosis in patients with NSCLC (47). However, after more than 15 years of research in this field, assessment of CTC did not enter in the routine clinical management of NSCLC patients.
A number of issues are indeed limiting the transfer of CTC count to the clinical scenario.
One of the major drawbacks is represented by the fact that several different methods and thresholds have been employed in studies of CTC detection in NSCLC, thus limiting the possibility to compare the findings of these analyses. Reproducibility and sensitivity of CTC detection is still a major issue. Automated systems for CTC isolation and identification such as the CellSearch warrant a higher standardization of the procedure. However, the use of an epithelial cell marker such as EpCam for CTC isolation might lead to an underestimation of the CTC count because of a potential loss of epithelial markers during the EMT that is a phenomenon frequently associated with the metastatic cascade (48). Methods that are more sensitive have been recently demonstrated to capture a higher number of CTC in NSCLC patients (12,49). Sensitivity of CTC detection is an important issue also for early diagnosis in high-risk patients as well as for prognostic assessment in early lung cancer. However, the sensitivity in these settings needs to be counterbalanced by an appropriate specificity in order to limit the false positive rate.
Several different studies have demonstrated that the detection of CTC in the pre-operative and/or post-operative period in early lung cancer patients correlate with tumor recurrence. Some studies suggest that the assessment of PV CTC might increase the sensitivity of detection of CTC and the predictive value of the analysis in this setting. In this respect, recent studies have demonstrated that detection of somatic mutation in the circulating free DNA (cfDNA) after surgery predicts tumor recurrence in early breast and colorectal carcinoma (50,51). Therefore, evaluation of minimal residual disease in early tumor stages might represent one of the most interesting fields of application of CTC in lung cancer in the next future.
Although several different trials have demonstrated a prognostic role of CTC count in patients with advanced NSCLC, few studies have confirmed these findings at the multivariate analysis (Tables 2,3). In addition, low numbers of patients have been enrolled in these studies conducted with different methods for CTC detection. Both qualitative methods assessing transcripts for epithelial markers as well as methods that allow isolation and quantification of CTC have been employed. The advantage of the latter techniques is that they permit to follow better the changes in CTC count during treatment, which might reflect the sensitivity of the tumor to chemotherapy. The utility of this information for the development of novel therapeutic strategies needs to be evaluated in prospective randomized clinical trials.
A number of studies have shown that CTC can be used for molecular profiling of the tumor and, in particular, for the identification of predictive biomarkers. For example, molecular alterations of EGFR, ALK and ROS1 are detectable in CTC isolated from NSCLC patients and they correspond to the mutational status of the primary tumor (52-57). However, we have to acknowledge that the field of molecular profiling of the tumor through liquid biopsy is currently dominated by the analysis of circulating tumor DNA (ctDNA). Indeed, ctDNA analysis has the advantage of lower costs and complexity for the extraction of tumor-derived nucleic acids as compared with CTC. In addition, the low number of CTC that are usually isolated in patients with NSCLC makes particularly complex the molecular analysis. Nevertheless, analysis of CTC has some advantages over ctDNA. First, analysis of CTC might allow the identification of protein biomarkers that cannot be revealed by analysis of nucleic acids. For example, CTC isolation can be optimized for the assessment of PD-L1 expression as potential biomarker of response to checkpoint inhibitors (58). Both analysis of ctDNA and CTC might result in false negative results due to the relative low sensitivity of these approaches. In this respect, it has been shown that contemporary analysis of CTC and ctDNA increases the possibility to detect predictive biomarkers in NSCLC patients, therefore improving the sensitivity of the liquid biopsy test (59). Finally, molecular profiling of single CTC might provide information on tumor heterogeneity that cannot be derived from ctDNA. Increasing evidence shows that the majority of solid tumors, including NSCLC, are highly heterogeneous (60,61). As a consequence of such intra-tumor heterogeneity, also driver mutations might be subclonal in selected patients (60,62,63). Evidence also suggests that the tumor heterogeneity is likely to increase over the time with the different lines of therapy. For example, significant fractions of patients that carry the T790M resistance mutations also have additional resistance mechanisms that can significantly affect the response to T790M inhibitors (64). In this scenario, analysis of single CTC will clear whether these molecular alterations occur in the same clone of neoplastic cells or in different clones, thus allowing the development of specific therapeutic strategies. The possibility to perform multiplex molecular profiling of single CTC up to RNAseq analysis will also allow deriving important information on tumor pathogenesis as well as on the mechanisms involved in tumor dissemination (65).
Recent studies have also demonstrated that CTC from lung cancer patients can be used to generate patient’s derived xenografts in immunocompromised mice also defined as xenopatients (48,66). Xenopatients are a valuable tool to gain information on the mechanisms regulating the formation of metastasis as well for studying the sensitivity or resistance to chemotherapeutics and to develop novel therapeutic strategies.
In conclusion, prospective clinical trials in adequate cohorts of patients are needed to confirm the prognostic and predictive value of CTC in NSCLC. Nevertheless, the study of CTC plays a fundamental role to gain novel information on the molecular evolution of the disease and to design novel therapeutic strategies in NSCLC.
Acknowledgements
We thank A. Trocino (INT-Fondazione Pascale, Naples, Italy) for bibliographic assistance.
Funding: This work was supported by a grant from the Associazione Italiana per la Ricerca sul Cancro (AIRC) to N. Normanno (grant number: IG17135).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Dotan E, Cohen SJ, Alpaugh KR, et al. Circulating tumor cells: evolving evidence and future challenges. Oncologist 2009;14:1070-82. [Crossref] [PubMed]
- Alix-Panabières C, Pantel K. Challenges in circulating tumour cell research. Nat Rev Cancer 2014;14:623-31. [Crossref] [PubMed]
- Alix-Panabières C, Pantel K. Clinical Applications of Circulating Tumor Cells and Circulating Tumor DNA as Liquid Biopsy. Cancer Discov 2016;6:479-91. [Crossref] [PubMed]
- Herbst RS, Heymach JV, Lippman SM. Lung cancer. N Engl J Med 2008;359:1367-80. [Crossref] [PubMed]
- Johnson DH, Schiller JH, Bunn PA Jr. Recent clinical advances in lung cancer management. J Clin Oncol 2014;32:973-82. [Crossref] [PubMed]
- Sheu CC, Yu YP, Tsai JR, et al. Development of a membrane array-based multimarker assay for detection of circulating cancer cells in patients with non-small cell lung cancer. Int J Cancer 2006;119:1419-26. [Crossref] [PubMed]
- Yu Y, Chen Z, Dong J, et al. Folate receptor-positive circulating tumor cells as a novel diagnostic biomarker in non-small cell lung cancer. Transl Oncol 2013;6:697-702. [Crossref] [PubMed]
- Wan JW, Gao MZ, Hu RJ, et al. A preliminary study on the relationship between circulating tumor cells count and clinical features in patients with non-small cell lung cancer. Ann Transl Med 2015;3:352. [PubMed]
- Wang L, Wu C, Qiao L, et al. Clinical Significance of Folate Receptor-positive Circulating Tumor Cells Detected by Ligand-targeted Polymerase Chain Reaction in Lung Cancer. J Cancer 2017;8:104-10. [Crossref] [PubMed]
- Hofman VJ, Ilie MI, Bonnetaud C, et al. Cytopathologic detection of circulating tumor cells using the isolation by size of epithelial tumor cell method: promises and pitfalls. Am J Clin Pathol 2011;135:146-56. [Crossref] [PubMed]
- Ilie M, Hofman V, Long-Mira E, et al. “Sentinel” circulating tumor cells allow early diagnosis of lung cancer in patients with chronic obstructive pulmonary disease. PloS one 2014;9:e111597. [Crossref] [PubMed]
- Gao W, Yuan H, Jing F, et al. Analysis of circulating tumor cells from lung cancer patients with multiple biomarkers using high-performance size-based microfluidic chip. Oncotarget 2017;8:12917-28. [PubMed]
- Sawabata N, Kitamura T, Nitta Y, et al. Lung cancer biopsy dislodges tumor cells into circulating blood. J Cancer Metastasis Treat 2017;3:16-20. [Crossref]
- Okumura Y, Tanaka F, Yoneda K, et al. Circulating Tumor Cells in Pulmonary Venous Blood of Primary Lung Cancer Patients. Ann Thorac Surg 2009;87:1669-75. [Crossref] [PubMed]
- Hashimoto M, Tanaka F, Yoneda K, et al. Significant increase in circulating tumour cells in pulmonary venous blood during surgical manipulation in patients with primary lung cancer†. Interact Cardiovasc Thorac Surg 2014;18:775-83. [Crossref] [PubMed]
- Reddy RM, Murlidhar V, Zhao L, et al. Pulmonary venous blood sampling significantly increases the yield of circulating tumor cells in early-stage lung cancer. J Thorac Cardiovasc Surg 2016;151:852-8. [Crossref] [PubMed]
- Crosbie PA, Shah R, Krysiak P, et al. Circulating Tumor Cells Detected in the Tumor-Draining Pulmonary Vein Are Associated with Disease Recurrence after Surgical Resection of NSCLC. J Thorac Oncol 2016;11:1793-7. [Crossref] [PubMed]
- Yamashita JI, Kurusu Y, Fujino N, et al. Detection of circulating tumor cells in patients with non-small cell lung cancer undergoing lobectomy by video-assisted thoracic surgery: a potential hazard for intraoperative hematogenous tumor cell dissemination. J Thorac Cardiovasc Surg 2000;119:899-905. [Crossref] [PubMed]
- de Bono JS, Scher HI, Montgomery RB, et al. Circulating tumor cells predict survival benefit from treatment in metastatic castration-resistant prostate cancer. Clin Cancer Res 2008;14:6302-9. [Crossref] [PubMed]
- Ge MJ, Shi D, Wu QC, et al. Observation of circulating tumour cells in patients with non-small cell lung cancer by real-time fluorescent quantitative reverse transcriptase-polymerase chain reaction in peroperative period. J Cancer Res Clin Oncol 2006;132:248-56. [Crossref] [PubMed]
- Sawabata N, Okumura M, Utsumi T, et al. Circulating tumor cells in peripheral blood caused by surgical manipulation of non-small-cell lung cancer: pilot study using an immunocytology method. Gen Thorac Cardiovasc Surg 2007;55:189-92. [Crossref] [PubMed]
- Rolle A, Gunzel R, Pachmann U, et al. Increase in number of circulating disseminated epithelial cells after surgery for non-small cell lung cancer monitored by MAINTRAC(R) is a predictor for relapse: A preliminary report. World J Surg Oncol 2005;3:18. [Crossref] [PubMed]
- Yamashita J, Matsuo A, Kurusu Y, et al. Preoperative evidence of circulating tumor cells by means of reverse transcriptase-polymerase chain reaction for carcinoembryonic antigen messenger RNA is an independent predictor of survival in non-small cell lung cancer: a prospective study. J Thorac Cardiovasc Surg 2002;124:299-305. [Crossref] [PubMed]
- Yie SM, Lou B, Ye SR, et al. Clinical significance of detecting survivin-expressing circulating cancer cells in patients with non-small cell lung cancer. Lung Cancer 2009;63:284-90. [Crossref] [PubMed]
- Yoon SO, Kim YT, Jung KC, et al. TTF-1 mRNA-positive circulating tumor cells in the peripheral blood predict poor prognosis in surgically resected non-small cell lung cancer patients. Lung Cancer 2011;71:209-16. [Crossref] [PubMed]
- Li J, Shi SB, Shi WL, et al. LUNX mRNA-positive cells at different time points predict prognosis in patients with surgically resected nonsmall cell lung cancer. Transl Res 2014;163:27-35. [Crossref] [PubMed]
- Hofman V, Bonnetaud C, Ilie MI, et al. Preoperative circulating tumor cell detection using the isolation by size of epithelial tumor cell method for patients with lung cancer is a new prognostic biomarker. Clin Cancer Res 2011;17:827-35. [Crossref] [PubMed]
- Hofman V, Ilie MI, Long E, et al. Detection of circulating tumor cells as a prognostic factor in patients undergoing radical surgery for non-small-cell lung carcinoma: comparison of the efficacy of the CellSearch Assay and the isolation by size of epithelial tumor cell method. Int J Cancer 2011;129:1651-60. [Crossref] [PubMed]
- Sienel W, Seen-Hibler R, Mutschler W, et al. Tumour cells in the tumour draining vein of patients with non-small cell lung cancer: detection rate and clinical significance. Eur J Cardiothorac Surg 2003;23:451-6. [Crossref] [PubMed]
- Bayarri-Lara C, Ortega FG, Cueto Ladron de Guevara A, et al. Circulating Tumor Cells Identify Early Recurrence in Patients with Non-Small Cell Lung Cancer Undergoing Radical Resection. PLoS One 2016;11:e0148659. [Crossref] [PubMed]
- Pelosi G, Fraggetta F, Pasini F, et al. Immunoreactivity for thyroid transcription factor-1 in stage I non-small cell carcinomas of the lung. Am J Surg Pathol 2001;25:363-72. [Crossref] [PubMed]
- Krebs MG, Sloane R, Priest L, et al. Evaluation and prognostic significance of circulating tumor cells in patients with non-small-cell lung cancer. J Clin Oncol 2011;29:1556-63. [Crossref] [PubMed]
- Muinelo-Romay L, Vieito M, Abalo A, et al. Evaluation of Circulating Tumor Cells and Related Events as Prognostic Factors and Surrogate Biomarkers in Advanced NSCLC Patients Receiving First-Line Systemic Treatment. Cancers 2014;6:153-65. [Crossref] [PubMed]
- Hirose T, Murata Y, Oki Y, et al. Relationship of circulating tumor cells to the effectiveness of cytotoxic chemotherapy in patients with metastatic non-small-cell lung cancer. Oncol Res 2012;20:131-7. [Crossref] [PubMed]
- Xu YH, Zhou J, Pan XF. Detecting circulating tumor cells in patients with advanced non-small cell lung cancer. Genet Mol Res 2015;14:10352-8. [Crossref] [PubMed]
- Juan O, Vidal J, Gisbert R, et al. Prognostic significance of circulating tumor cells in advanced non-small cell lung cancer patients treated with docetaxel and gemcitabine. Clin Transl Oncol 2014;16:637-43. [Crossref] [PubMed]
- Tarumi S, Gotoh M, Kasai Y, et al. Innovative method using circulating tumor cells for prediction of the effects of induction therapy on locally advanced non-small cell lung cancer. J Cardiothorac Surg 2013;8:175. [Crossref] [PubMed]
- Punnoose EA, Atwal S, Liu W, et al. Evaluation of circulating tumor cells and circulating tumor DNA in non-small cell lung cancer: association with clinical endpoints in a phase II clinical trial of pertuzumab and erlotinib. Clin Cancer Res 2012;18:2391-401. [Crossref] [PubMed]
- Isobe K, Hata Y, Kobayashi K, et al. Clinical significance of circulating tumor cells and free DNA in non-small cell lung cancer. Anticancer Res 2012;32:3339-44. [PubMed]
- Zhang Z, Xiao Y, Zhao J, et al. Relationship between circulating tumour cell count and prognosis following chemotherapy in patients with advanced non-small-cell lung cancer. Respirology 2016;21:519-25. [Crossref] [PubMed]
- Du YJ, Li J, Zhu WF, et al. Survivin mRNA-circulating tumor cells predict treatment efficacy of chemotherapy and survival for advanced non-small cell lung cancer patients. Tumour Biol 2014;35:4499-507. [Crossref] [PubMed]
- Nieva J, Wendel M, Luttgen MS, et al. High-definition imaging of circulating tumor cells and associated cellular events in non-small cell lung cancer patients: a longitudinal analysis. Phys Biol 2012;9:016004. [Crossref] [PubMed]
- Liu L, Liao GQ, He P, et al. Detection of circulating cancer cells in lung cancer patients with a panel of marker genes. Biochem Biophys Res Commun 2008;372:756-60. [Crossref] [PubMed]
- Sher YP, Shih JY, Yang PC, et al. Prognosis of non-small cell lung cancer patients by detecting circulating cancer cells in the peripheral blood with multiple marker genes. Clin Cancer Res 2005;11:173-9. [PubMed]
- Chen TF, Jiang GL, Fu XL, et al. CK19 mRNA expression measured by reverse-transcription polymerase chain reaction (RT-PCR) in the peripheral blood of patients with non-small cell lung cancer treated by chemo-radiation: an independent prognostic factor. Lung Cancer 2007;56:105-14. [Crossref] [PubMed]
- He W, Li W, Jiang B, et al. Correlation between epidermal growth factor receptor tyrosine kinase inhibitor efficacy and circulating tumor cell levels in patients with advanced non-small cell lung cancer. Onco Targets Ther 2016;9:7515-20. [Crossref] [PubMed]
- Wang J, Wang K, Xu J, et al. Prognostic Significance of Circulating Tumor Cells in Non-Small-Cell Lung Cancer Patients: A Meta-Analysis. Plos One 2013;8:e78070. [Crossref] [PubMed]
- Morrow CJ, Trapani F, Metcalf RL, et al. Tumourigenic non-small-cell lung cancer mesenchymal circulating tumour cells: a clinical case study. Ann Oncol 2016;27:1155-60. [Crossref] [PubMed]
- Gorges TM, Penkalla N, Schalk T, et al. Enumeration and Molecular Characterization of Tumor Cells in Lung Cancer Patients Using a Novel In Vivo Device for Capturing Circulating Tumor Cells. Clin Cancer Res 2016;22:2197-206. [Crossref] [PubMed]
- Garcia-Murillas I, Schiavon G, Weigelt B, et al. Mutation tracking in circulating tumor DNA predicts relapse in early breast cancer. Sci Transl Med 2015;7:302ra133. [Crossref] [PubMed]
- Tie J, Wang Y, Tomasetti C, et al. Circulating tumor DNA analysis detects minimal residual disease and predicts recurrence in patients with stage II colon cancer. Sci Transl Med 2016;8:346ra92. [Crossref] [PubMed]
- Maheswaran S, Sequist LV, Nagrath S, et al. Detection of mutations in EGFR in circulating lung-cancer cells. N Engl J Med 2008;359:366-77. [Crossref] [PubMed]
- Ilie M, Long E, Butori C, et al. ALK-gene rearrangement: a comparative analysis on circulating tumour cells and tumour tissue from patients with lung adenocarcinoma. Ann Oncol 2012;23:2907-13. [Crossref] [PubMed]
- Pailler E, Adam J, Barthelemy A, et al. Detection of circulating tumor cells harboring a unique ALK rearrangement in ALK-positive non-small-cell lung cancer. J Clin Oncol 2013;31:2273-81. [Crossref] [PubMed]
- Pailler E, Auger N, Lindsay CR, et al. High level of chromosomal instability in circulating tumor cells of ROS1-rearranged non-small-cell lung cancer. Ann Oncol 2015;26:1408-15. [Crossref] [PubMed]
- Tan CL, Lim TH, Lim T, et al. Concordance of anaplastic lymphoma kinase (ALK) gene rearrangements between circulating tumor cells and tumor in non-small cell lung cancer. Oncotarget 2016;7:23251-62. [Crossref] [PubMed]
- He W, Xu D, Wang Z, et al. Detecting ALK-rearrangement of CTC enriched by nanovelcro chip in advanced NSCLC patients. Oncotarget 2016. [Epub ahead of print].
- Schehr JL, Schultz ZD, Warrick JW, et al. High Specificity in Circulating Tumor Cell Identification Is Required for Accurate Evaluation of Programmed Death-Ligand 1. PLoS One 2016;11:e0159397. [Crossref] [PubMed]
- Sundaresan TK, Sequist LV, Heymach JV, et al. Detection of T790M, the Acquired Resistance EGFR Mutation, by Tumor Biopsy versus Noninvasive Blood-Based Analyses. Clin Cancer Res 2016;22:1103-10. [Crossref] [PubMed]
- McGranahan N, Favero F, de Bruin EC, et al. Clonal status of actionable driver events and the timing of mutational processes in cancer evolution. Sci Transl Med 2015;7:283ra54. [Crossref] [PubMed]
- Andor N, Graham TA, Jansen M, et al. Pan-cancer analysis of the extent and consequences of intratumor heterogeneity. Nat Med 2016;22:105-13. [Crossref] [PubMed]
- Normanno N, Rachiglio AM, Lambiase M, et al. Heterogeneity of KRAS, NRAS, BRAF and PIK3CA mutations in metastatic colorectal cancer and potential effects on therapy in the CAPRI GOIM trial. Ann Oncol 2015;26:1710-4. [Crossref] [PubMed]
- Rachiglio AM, Esposito Abate R, Sacco A, et al. Limits and potential of targeted sequencing analysis of liquid biopsy in patients with lung and colon carcinoma. Oncotarget 2016;7:66595-605. [Crossref] [PubMed]
- Normanno N, Maiello MR, Chicchinelli N, et al. Targeting the EGFR T790M mutation in non-small-cell lung cancer. Expert Opin Ther Targets 2017;21:159-65. [Crossref] [PubMed]
- Miyamoto DT, Zheng Y, Wittner BS, et al. RNA-Seq of single prostate CTCs implicates noncanonical Wnt signaling in antiandrogen resistance. Science 2015;349:1351-6. [Crossref] [PubMed]
- Hodgkinson CL, Morrow CJ, Li Y, et al. Tumorigenicity and genetic profiling of circulating tumor cells in small-cell lung cancer. Nat Med 2014;20:897-903. [Crossref] [PubMed]


